Blepharophimosis Syndrome
(Also known as Blepharophimosis Epicanthus Inversus Syndrome,
BPEI Syndrome, or BPES)
Author: Alon Kahana, MD, PhD
Kellogg Eye Center, University of Michigan
What is it?
Blepharophimosis syndrome is a genetic condition that presents at birth with:
- Horizontal narrowing of the eye opening (blepharophimosis)
- Drooping of the upper eyelids (blepharoptosis)
- Upward folding of skin from the lower eyelid at the inner corner of the eye (epicanthus inversus)
- Outward shifting of the inner corners (canthi) of the eyes (telecanthus)
- Within these canthi are the tear ducts, which might be disfigured due to the telecanthus, causing excessive tearing because of defective drainage of tears
- Downward shifting of the outer corners of the lower eyelids (euryblepharon)
All of these characteristics together result in an inability to properly open the eyes to clear the visual axis, and as a result may significantly impact vision – particularly during early childhood visual development.
Often, patients will demonstrate a significant “chin-up” position (also known as “ocular torticollis”) in order to see from uder the eyelids – a situation that can place significant stress on the neck and back and can delay gross motor development in infants and toddlers.
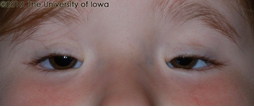
A patient with BPES. Note that a corneal light reflex from the flash can be just barely seen in the right eye just below the eyelid margin, but cannot be seen in the left eye, indicating obstruction of the visual axis that is worse on the left.
(http://webeye.ophth.uiowa.edu/eyeforum/cases-i/case114/larger/3-Blepharophimosis.jpg)
There are two types of Blepharophimosis Syndrome:
- Type I is associated with early menopause along with the aforementioned eyelid characteristics above. This can lead to increased difficulty, or complete inability, to conceive children.
- Type II only includes the eyelid characteristics mentioned above.
Blepharophimosis syndrome does not impact intellectual development in any way. However, a negative impact on visual development can lead to vision disabilities.
What Causes It?
A mutation in the gene FOXL2 is known to be associated with this syndrome. FOXL2 is a gene that is expressed in several areas in the body, including the eyelids and ovaries. Those with the genetic mutation have a 50% chance of passing it on to their offspring. Other genetic mutations are also known to be associated with this syndrome.
Treatment and Management
This is a condition that requires the input of several specialists, including ophthalmologists, endocrinologists, gynecologists, and geneticists.
The first and most important step is to have a complete eye exam performed by a fellowship-trained pediatric ophthalmologist, who is a medical doctor (MD’s or DO’s with specialized training in both vision medicine and pediatric optics). Only fellowship-trained pediatric ophthalmologists have the skills necessary to assess vision in infants and toddlers. It is also critical to assess for common but unrelated vision issues, such as strabismus (eye misalignment) and refractive error (the need for glasses). The fact that a child has blepharophimosis should not distract from the need to take care of ANY and ALL vision-related issues that commonly arise in young children.
The eyelid manifestations of blepharophimosis syndrome require surgical correction, typically done by an ophthalmologist with specialized fellowship training in oculoplastic surgery.
The primary goal of surgical repair is to facilitate normal development of the visual system and to avoid the consequences of neck strain caused by a “chin-up” position (ocular torticollis). If visual development is normal then there is NO REASON to operate on a young child. The only reason to operate on an infant or toddler, in whom surgery is more challenging, is to normalize visual development and/or correct the ocular torticollis. If surgery can be delayed until school age, then it should be delayed in order to optimize long-term results.
Surgery is performed in stages, starting either with the blepharoptosis (to raise the upper eyelid – ptosis correction) or with the epicanthus inversus and telecanthus (to reduce the inner skin folds – medial canthoplasty). The decision on which surgery to perform first is individualized and takes into account which part of the lid – upper and inner – might be obstructing vision.
The medial canthoplasty is performed by moving skin flaps to reorient the tissues such that the inner skin folds will be pulled inward. In addition, debulking of abnormal medial canthal fat pads is necessary to narrow the nasal bridge to a more anatomically correct position. Care must be taken to avoid injury to the tear drainage (lacrimal) system.
The blepharoptosis repair surgery aims to allow the upper eyelid to elevate better in order to clear the pupil without a chin lift. There are two methods to correct this, depending on the severity:
- If the typical muscle that normally elevate the eyelid, called the levator palpebrae superioris muscle, has sufficient muscle function, then a levator muscle operation is performed.
- Most patients with BPES, however, have very poor function of their levator muscles. In this case, the best option is to do a frontalis sling operation.
- In this surgery, the frontalis muscle, located in the forehead to raise the eyebrows, is attached to the upper eyelid, thus allowing for eyelid control through movement of the brow.
- To connect the frontalis muscle to the eyelid, traditional surgery utilizes one of several methods: silicone tubing, Gortex suture, connective tissue from the thigh (fascia lata), or cadaveric connective tissue from a tissue bank.
- After many years of using silicone slings, Dr. Kahana has revised and improved on an old technique in which the frontalis muscle itself is tunneled under the brow and connected to the upper eyelid – forgoing the need for an implant. This technique is called a “frontalis muscle flap sling.” (Credit goes to Dr. Suzana Matayoshi, MD, PhD, Director of Oculoplastic Surgery at the University of Sao Paolo, Brazil, for introducing Dr. Kahana to this approach.)
- In many patients, it is worthwhile to perform BOTH levator surgery and a frontalis sling, and this combination provides the best overall result. Combining both techniques is a tricky operation that should be performed by an experienced pediatric oculoplastic surgeon.
- After surgery, the eyelids will be more open, but they will not close as well when the patient is asleep – at least for the first 2-3 weeks. They will also not blink as well because the blinking mechanism is altered by the sling surgery and needs time to recover. Therefore, it is very important that the eyes are kept lubricated – particularly when sleeping. This is done by applying a small amount of eye lubricating ointment to the eyes whenever the child is asleep (including naps). Drying out of the eyes is the most important early complication to avoid – it can lead to corneal infection, scarring and loss of vision. In infants and pre-verbal toddlers, rubbing of the eyes is often a sign that the eyes are dry and uncomfortable. Fortunately, the issue is usually temporary and improves as the eyelids heal over a few weeks after surgery, although prolonged swelling is possible – particularly with traditional silicone or fascia lata slings.
Again – the TIMING of surgery is really driven by visual development as determined by a pediatric ophthalmologist. This important point warrants additional discussion.
CRITICAL PERIOD OF VISUAL DEVELOPMENT:
At birth, vision is not fully developed, and a newborn’s visual acuity is relatively poor. Children’s ability to see improves dramatically over the first 7 years of life, and particularly in the first 2-3 years – the “critical phase of visual development.” Visual development is driven by brain development in the visual cortex and vision processing centers in the brain. Development of those parts of the brain required for good vision occurs with visual input from the child’s eyes. In Nobel Prize-winning work, Professors David Hubel and Torsten Wiesel of the Johns Hopkins University showed that brain development REQUIRED visual input from the eyes (see https://youtu.be/IOHayh06LJ4). If visual input was impaired, e.g. eyelids covering the visual axis, then the brain would not develop the ability to see well. Importantly, there is a CRITICAL PERIOD of brain development in which the brain can develop the ability to see well. If the visual axis (i.e. pupil) is covered during this time then the brain will never develop the ability to see well – EVEN AFTER THE OBSTRUCTION IS REMOVED. Hence, it is very important – even critical – to have a good assessment of visual function by a fellowship-trained pediatric ophthalmologist, and to take this issue into account when deciding on when to perform eyelid surgery.
Dr. Kahana recommends that the evaluation of visual function be performed by a fellowship-trained pediatric ophthalmologist (MD or DO), not an optometrist or pediatric optometrist (OD). This is because MDs and DOs are medical doctors with surgical training and comprehensive training in ophthalmology, including the neurologic circuits of vision. Pediatric optometrists can be very valuable members of the care team, but in Dr. Kahana’s opinion their skill set is not well-suited to the primary evaluation of infant patients with complex congenital or genetic eye disorders.
Girls with Blepharophimosis syndrome should be assessed by an endocrinologist and gynecologist for potential early menopause and fertility concerns.
It is very important to see a geneticist for genetic counseling, who can help discuss the risk of passing this on to future generations, along with assessing the risk for early menopause.
Outcome
As long as the eyelids are properly repaired in a timely fashion and there is appropriate follow-up, patients with blepharophimosis syndrome are expected to develop normal vision.
Acknowledgements: Dr. Kahana would like to thank Amr Sabbagh (MS4, University of Michigan) for his assistance, and Dr. Brenda Bohnsack and Dr. Grace Wang at the University of Michigan for critical reading and helpful comments.
Click here to download a pdf version of this information
